A nurse caring for patients with COVID 19.
A day in my life as a critical care nurse with carrying for patients with coronavirus, My work shift is typically 0700 am- 07:30 PM. A long 12 almost 13 hour day.
Prior to work, I go to a website link on my phone and fill out a questionnaire asking if I have any symptoms which include,
fever 99°F
chills
muscles aches
cough
shortness of breathe
unexpected fatigue
sore throat
loss of taste or smell
headache
diarrhea
vomiting/nausea
or other cold symptoms.
After checking off none of the above, then i will receive a green check mark for the okay to proceed to work.
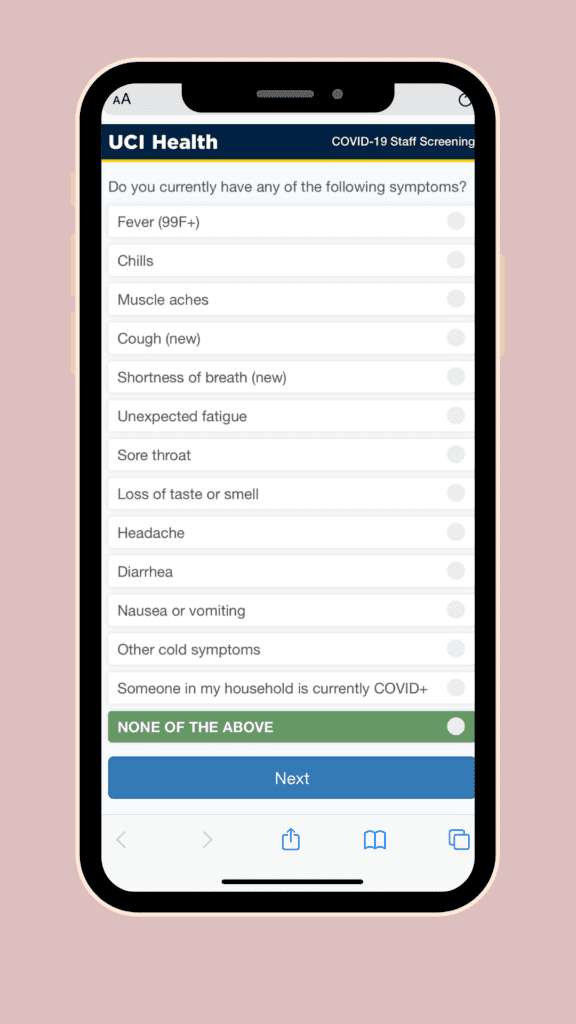
Next, there are only certain entrances that my hospital has open. From those specific entrances, we may have to wait outside in a line, maintaining a 6 foot distance, to get our temperatures taken before coming into work. You must also have a mask on prior to walking into work. The screeners will ask if we have any symptoms and take our temperature. Any temperature above 99.0°F the employee would have to go to occupational health. After passing the with screener, and showing them your phone confirmation you receive a wrist band. Everyday is a different color that you then will loop around your badge so everyone is able to see it.

After passing the check point, I typically go and get a pair of surgical scrubs. The hospital offers clean scrubs to all employees, for our comfort level as well as to maintain at least contamination as possible. Currently, you can sign out one pair of scrubs and then return them dirty at the end of the day. They provide you a surgical top and a pair of pants, as well as a linen bag for returning the dirty scrubs. For some people working a few days in a row, they will let you check out a pair the night before, so you don’t have to change the morning of, at the hospital.
After changing into new scrubs, it’s time to go to morning huddle. Prior to COVID-19, we held the morning huddle in the break rooms. Due to social distancing, we now do morning huddles in the hallways. Typically the charge nurse will be there with report, the nursing assignment, and to hand out masks. Employees who are using the N95 mask, must sign them out by writing down their name and size (small or medium). If I have a COVID patient, I will sign out an N95 as well as a surgical mask, with small clear Ziploc bags or brown paper lunch bags. On the Ziploc bags, I put my name and when Im not wearing either the N95 or the surgical mask, I am to keep it in the plastic bag.
After morning huddle, it’s finally time to start the shift by getting the report from the night nurse. Currently with all covid patients, we are doing report outside of the room. The hospital is not allowing visitors at this time due to the COVID pandemic, but is helpful during this stressful time and extra speculations for the staff members.
Before entering the room to care for my positive COVID-19 patient or any other COVID-19 rule out patients, (a patient under investigation for COVID-19) it is my duty as the nurse to properly don personal protective equipment (PPE). The process needs to be methodically and efficient when applying the gloves, gown, mask, and face shields. It is definitely a process prior to going into the room. As a nurse we emphasize the importance of clustered care. Clustered care meaning to limit the amount of times the nurse goes in and out of the room. We have been practicing clustered care in nursing forever, however this time it’s more vital due to the amount of Personal Protective Equipment (PPE). So typically before going into my patient’s room and gowning up, I try to make sure I have everything I need before starting my care. This would include, saline flushes, medications, linen, mouth swabs, suction equipment, alcohol swabs, etc.Outside of the room we also have an observe, runner, helper a person designated to monitor proper application of PPE, as well as to help out. That way if we forget something for the room, we poke our heads out and ask them or someone else to grab it for us. However, when wearing an N95 mask and all this equipment, its very difficult for people to hear and understand you. Sometimes we will use a white board to write our messages on and than share them through the glass door to communicate with them.
Inside the room, we then are able to do our nursing care. I can say wearing an eye shield or protective glasses, it can get frustrating when the screen fogs up making it more difficult to see. Also, you feel a bit claustrophobic and suffocated wearing all this equipment while trying to do your nursing roles. Sometimes your phone rings, or family members are asking us to facetime with the patients so they can see their loved ones. I also feel awful for the patients in the room. They must feel like we don’t want to be around them. As a nurse its important to build a relationship with our patients and to gain a rapport. During this time we our very limited to what we can do with all the extra steps and restrictions it can be very overwhelming and frustrating.
However, I think it is sinking into healthcare workers and to society that this is going to be the new norm for a while. I am beyond grateful for my job, and being able to work with so many amazing healthcare workers and keep a positive attitude. This is just a little peak inside my world as a critical care nurse caring for COVID-19 patients. And trust me there are a lot more details that go into it.









8 Comments
You made fun of the side effects after getting the Covid 19 shot on TikTok. That was inexcusable especially since you are a nurse! 😡😡
Thank you so much for your hard work! I appreciate you sharing a peek into your day 🙂
This was such an interesting read! Thank you for sharing what it’s like, and thank you for taking care of people ❤️
Thanks so much for your service! So thankful for you and the other front line providers.
Your post was eye opening. I am so grateful for what you do. I am so grateful for what all people in the health care field do to take care of us during this crazy time.
Thanks for taking us inside your day and thanks for all that you do! I am a nurse in primary care and we do daily COVID testing here. It’s such a hard time for everyone ❤️
Love your new blog. So proud of all your achievements.